Search
- Page Path
- HOME > Search
Original Article
- Clinical characteristics and prognosis of Korean patients with hepatocellular carcinoma with respect to etiology
- Wonjoon Jang, Hye Won Lee, Jae Seung Lee, Beom Kyung Kim, Seung Up Kim, Jun Yong Park, Sang Hoon Ahn, Do Young Kim
- J Liver Cancer. 2022;22(2):158-166. Published online September 27, 2022
- DOI: https://doi.org/10.17998/jlc.2022.09.18

- 2,770 Views
- 66 Downloads
- 7 Citations
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background/Aim
The profile of patients with hepatocellular carcinoma (HCC) has changed globally; the role of etiology in predicting prognosis of HCC patients remains unclear. We aimed to analyze the characteristics and prognosis of Korean patients with HCC according to disease etiology.
Methods
This retrospective observational study included patients diagnosed with HCC between 2010 and 2014 in a single center in Korea. Patients with HCC aged <19 years old, had coinfection with other viral hepatitis, had missing follow-up data, were Barcelona Clinic Liver Cancer stage D, or died before 1 month were excluded.
Results
A total of 1,595 patients with HCC were analyzed; they were classified into the hepatitis B virus (HBV) group (1,183 [74.2%]), hepatitis C virus (HCV) group (146 [9.2%]), and non-B non-C (NBNC) group (266 [16.7%]). The median overall survival of all patients was 74 months. The survival rates at 1, 3, and 5 years were 78.8%, 62.0% and 54.9% in the HBV group; 86.0%, 64.0%, and 48.6% in the HCV group; and 78.4%, 56.5%, and 45.9% in the NBNC group, respectively. NBNC-HCC has a poorer prognosis than other causes of HCC. Survival was significantly longer in the HBV group with early-stage HCC than in the NBNC group. Furthermore, survival was shorter in patients with early-stage HCC and diabetes mellitus (DM) than in those without DM.
Conclusions
The etiology of HCC affected clinical characteristics and prognosis to some extent. NBNC-HCC patients showed shorter overall survival than viral-related HCC patients. Additionally, the presence of DM is an additional important prognostic factor in patients with early-stage HCC. -
Citations
Citations to this article as recorded by- The Epidemiology of Hepatitis B Virus Infection in Korea: 15-Year Analysis
Log Young Kim, Jeong-Ju Yoo, Young Chang, Hoongil Jo, Young Youn Cho, Sangheun Lee, Dong Hyeon Lee, Jae Young Jang
Journal of Korean Medical Science.2024;[Epub] CrossRef - Comparison of Surgical Resection and Radiofrequency Ablation in Elderly Patients with Hepatocellular Carcinoma
Jun Il Kim, Jayoun Lee, Gi Hong Choi, Min Woo Lee, Dong Ah Park, Jeong-Ju Yoo
Digestive Diseases and Sciences.2024; 69(3): 1055. CrossRef - Focal Segmental Glomerulosclerosis Followed by Acute Hepatitis A Infection: Case Report
Min-Woo An, Jeong-Ju Yoo, Jin Kuk Kim, Ahrim Moon, Sang Gyune Kim, Young Seok Kim
Medicina.2023; 59(5): 819. CrossRef - Validation of MELD 3.0 scoring system in East Asian patients with cirrhosis awaiting liver transplantation
Jeong-Ju Yoo, Jong-In Chang, Ji Eun Moon, Dong Hyun Sinn, Sang Gyune Kim, Young Seok Kim
Liver Transplantation.2023; 29(10): 1029. CrossRef - A nationwide study on the current treatment status and natural prognosis of hepatocellular carcinoma in elderly
Jeong-Ju Yoo, Jayoun Lee, Gi Hong Choi, Min Woo Lee, Dong Ah Park
Scientific Reports.2023;[Epub] CrossRef - Statin use and the risk of hepatocellular carcinoma among patients with chronic hepatitis B: an emulated target trial using longitudinal nationwide population cohort data
Dong Hyun Sinn, Danbee Kang, Yewan Park, Hyunsoo Kim, Yun Soo Hong, Juhee Cho, Geum-Youn Gwak
BMC Gastroenterology.2023;[Epub] CrossRef - Addition of Kidney Dysfunction Type to MELD-Na for the Prediction of Survival in Cirrhotic Patients Awaiting Liver Transplantation in Comparison with MELD 3.0 with Albumin
Kyeong-Min Yeom, Jong-In Chang, Jeong-Ju Yoo, Ji Eun Moon, Dong Hyun Sinn, Young Seok Kim, Sang Gyune Kim
Diagnostics.2023; 14(1): 39. CrossRef
- The Epidemiology of Hepatitis B Virus Infection in Korea: 15-Year Analysis

Case Report
- A Case of Lymphocyte-Rich Hepatocellular Carcinoma in a Patient Who Was Treated for Colon Cancer
- Jae Won Song, Ho Soo Chun, Jae Seung Lee, Hye Won Lee, Beom Kyung Kim, Seung Up Kim, Jun Yong Park, Sang Hoon Ahn, Young Nyun Park, Dai Hoon Han, Do Young Kim
- J Liver Cancer. 2021;21(1):69-75. Published online March 31, 2021
- DOI: https://doi.org/10.17998/jlc.21.1.69
- 3,543 Views
- 84 Downloads
- 2 Citations
-
 Abstract
Abstract
 PDF
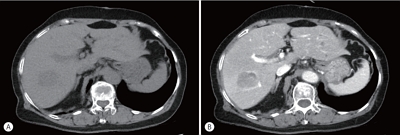
PDF - Hepatocellular carcinoma (HCC) primarily originates in the liver with hepatic differentiation. However, HCCs are not homogenous, and approximately 35% of HCC cases are classified as histopathological variants that present distinct pathologic characteristics. In particular, the lymphocyte-rich variant is the rarest subtype accounting for less than 1% of HCCs, which is not well known to date about molecular features and pathophysiology. Herein, we present a case of a patient who was suspected of metastatic liver cancer and confirmed as lymphocyte-rich HCC pathologically. A 78-year-old woman who underwent a right hemicolectomy for colon cancer was referred to our hospital for a newly detected liver mass. We could not make a decision because of insufficient evidence for diagnosis from imaging studies. After resection, we found that it was a lymphocyte-rich HCC. The pathologic features and prognostic trends of this subtype are also discussed.
-
Citations
Citations to this article as recorded by- Characterization of lymphocyte‐rich hepatocellular carcinoma and the prognostic role of tertiary lymphoid structures
Bokyung Ahn, Hee‐Sung Ahn, Jinho Shin, Eunsung Jun, Eun‐Young Koh, Yeon‐Mi Ryu, Sang‐Yeob Kim, Chang Ohk Sung, Ju Hyun Shim, JeongYeon Hong, Kyunggon Kim, Hyo Jeong Kang
Liver International.2024; 44(5): 1202. CrossRef - Uncommon variants of hepatocellular carcinoma: Not one size fits all
Reetu Kundu, Nalini Gupta, Debajyoti Chatterjee, Ajay Duseja
Diagnostic Cytopathology.2022; 50(1): 28. CrossRef
- Characterization of lymphocyte‐rich hepatocellular carcinoma and the prognostic role of tertiary lymphoid structures

Original Article
- Serum PD-1 Levels Change with Immunotherapy Response but Do Not Predict Prognosis in Patients with Hepatocellular Carcinoma
- Hye Won Lee, Kyung Joo Cho, Soon Young Shin, Ha Yan Kim, Eun Ju Lee, Beom Kyung Kim, Seung Up Kim, Jun Yong Park, Do Young Kim, Sang Hoon Ahn, Kwang-Hyub Han
- J Liver Cancer. 2019;19(2):108-116. Published online September 30, 2019
- DOI: https://doi.org/10.17998/jlc.19.2.108

- 5,377 Views
- 151 Downloads
- 5 Citations
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material - Background/Aim
s: Programmed death receptor 1 (PD-1) is a promising new target for treatment of patients with hepatocellular carcinoma (HCC). A high expression level of programmed death-ligand 1 (PD-L1) is a possible prognostic indicator for poor outcome in other malignancies. Here, we investigated the clinical significance of PD-1 and PD-L1 in patients with HCC.
Methods
We enrolled patients with HCC who underwent surgical resection at Severance Hospital between 2012 and 2017 and investigated the levels of PD-L1 in HCC tissues (tPD-L1) and PD-L1/PD-1 in serum (sPD-L1/sPD-1). We also aimed to determine whether expression levels correlated with clinical and histological features.
Results
A total of 72 patient samples were analyzed. The median sPD-L1 and sPD-1 levels were 25.72 and 341.44 pg/mL, respectively. A positive correlation was detected between tPD-L1 and sPD-1 levels (R2=0.426, P<0.001). The median sPD-1 level increased linearly with tPD-L1 score (P=0.002). During the follow-up period, HCC recurred in eight (11.1%) patients and liverrelated mortality occurred in eight (11.1%) patients. Higher sPD-L1 levels (≥19.18 pg/mL) tended to be associated with liver-related mortality (hazard ratio 6.866; 95% confidence interval, 0.804-58.659, P=0.078). sPD-1 levels of patients treated with nivolumab as a second-line therapy changed serially, and a >50% reduction in sPD-1 levels was observed immediately after nivolumab administration. However, sPD-1 level was not associated directly with prognosis in patients with advanced HCC.
Conclusions
The results demonstrated that PD-L1 and PD-1 levels changed according to the immunotherapy. However, no significant association with clinical outcome in patients with HCC was detected. -
Citations
Citations to this article as recorded by- Blood-based biomarkers for immune-based therapy in advanced HCC: Promising but a long way to go
Pil Soo Sung, Isaac Kise Lee, Pu Reun Roh, Min Woo Kang, Jaegyoon Ahn, Seung Kew Yoon
Frontiers in Oncology.2022;[Epub] CrossRef - Serum levels of soluble programmed death-ligand 1 (sPD-L1): A possible biomarker in predicting post-treatment outcomes in patients with early hepatocellular carcinoma
Tudor Mocan, Maria Ilies, Iuliana Nenu, Rares Craciun, Adelina Horhat, Ruxandra Susa, Iulia Minciuna, Ioana Rusu, Lavinia-Patricia Mocan, Andrada Seicean, Cristina Adela Iuga, Nadim Al Hajjar, Mihaela Sparchez, Daniel-Corneliu Leucuta, Zeno Sparchez
International Immunopharmacology.2021; 94: 107467. CrossRef - Interfacial interactions of SERS-active noble metal nanostructures with functional ligands for diagnostic analysis of protein cancer markers
Han-Jung Ryu, Won Kyu Lee, Yoon Hyuck Kim, Jae-Seung Lee
Microchimica Acta.2021;[Epub] CrossRef - Current Status and Future Direction of Immunotherapy in Hepatocellular Carcinoma: What Do the Data Suggest?
Hye Won Lee, Kyung Joo Cho, Jun Yong Park
Immune Network.2020;[Epub] CrossRef - Nivolumab for Advanced Hepatocellular Carcinoma with Multiple Lung Metastases after Sorafenib Failure
Jaewoong Kim, Jin Won Chang, Jun Yong Park
Journal of Liver Cancer.2020; 20(1): 72. CrossRef
- Blood-based biomarkers for immune-based therapy in advanced HCC: Promising but a long way to go

Case Reports
- A Case of Rapidly Recurred Hepatocellular Carcinoma with Distant Metastasis after Surgical Resection
- Mi Yeon Kim, Hye Won Lee, Kyu Sik Jung, Beom Kyung Kim, Seung Up Kim, Jun Yong Park, Sang Hoon Ahn, Kwang-Hyub Han, Do Young Kim
- J Liver Cancer. 2015;15(2):136-139. Published online September 30, 2015
- DOI: https://doi.org/10.17998/jlc.15.2.139
- 891 Views
- 7 Downloads
-
 Abstract
Abstract
 PDF
PDF - Hepatocellular carcinoma (HCC) is one of the cancers with poor prognosis. However, surgical resection is the treatment of choice as curative aim for early HCC with preserved liver function. A 5 year survival rate after curative resection is over 50%. We experienced a case of rapidly recurred HCC with bone metastasis after surgical resection. In our case, microscopically microvessel invasion was present after resection. Microvascular invasion (MVI) is an important factor to influence survival and/or HCC recurrence. So we suggested the patients with MVI need to follow up intensively and adjuvant therapy may be considered.

- A Case of Positive Tumor Marker Response after Intra-arterial Deferoxamine Infusion Therapy in a Hepatocellular Carcinoma Patient with Decompensated Liver Function
- Hyun Ju Kim, Wonseok Kang, Mi Na Kim, Beom Kyung Kim, Seung Up Kim, Do Young Kim, Sang Hoon Ahn, Kwang-Hyub Han
- J Liver Cancer. 2014;14(2):127-130. Published online September 30, 2014
- DOI: https://doi.org/10.17998/jlc.14.2.127
- 1,119 Views
- 6 Downloads
-
 Abstract
Abstract
 PDF
PDF - Treatment of hepatocellular carcinoma is often very challenging when the underlying liver function is decompensated. Recent experimental and clinical studies showed that some chelating agents, including deferoxamine, display anti-proliferative actions against tumor cells, thereby exhibiting anti-cancer effect in certain cancers, including hepatocellular carcinoma. Based on previous studies, we herein offer our experience of positive tumor marker response after intra-arterial deferoxamine infusion in a patient presenting with advanced hepatocellular carcinoma with decompensated hepatic function. Validation of the efficacy of intra-arterial deferoxamine therapy in the setting of advanced hepatocellular carcinoma with underlying decompensated hepatic function is warranted. (J Liver Cancer 2014;14:127-130)

- A Case of Partial Response of Hepatocellular Carcinoma Induced by Concurrent Chemoradiation and Hepatic Arterial Infusion Chemotherapy after Trans-Arterial Chemoembolization
- Myung Eun Song, Sangheun Lee, Mi Na Kim, Dong-Jun Lee, Beom Kyung Kim, Seung Up Kim, Jun Yong Park, Sang Hoon Ahn, Chae Yoon Chon, Kwang-Hyub Han, Jinsil Seong, Do Young Kim
- Journal of the Korean Liver Cancer Study Group. 2013;13(2):152-157. Published online September 30, 2013
- DOI: https://doi.org/10.17998/jlc.13.2.152
- 948 Views
- 7 Downloads
-
 Abstract
Abstract
 PDF
PDF - A 63-year-old man patient was referred for treatment of infiltrative hepatocellular carcinoma with hilar invasion after transarterial chemoembolization. Serum alkaline phosphatase and bilirubin were elevated, liver dynamic CT showed infiltrative type mass in left hepatic lobe and right hepatic dome with hilar invasion and left intrahepatic duct dilatation. Also CT showed obliteration of left portal vein and metastasis of lymph node around common bile duct. He was diagnosed as hepatocellular carcinoma (UICC stage IV-A, BCLC stage C). With the percutaneous transhepatic biliary drainage and the concurrent chemoradiation therapy and the 4th cycle of hepatic arterial infusion chemotherapy for infiltrative mass, viable tumor was decreased in resectable size at eight months from initial diagnosis.

- A Case of Recurred Hepatocellular Carcinoma after Treated by Trans-Arterial Chemoembolization
- Sangheun Lee, Mi Na Kim, Young Eun Chon, Beom Kyung Kim, Seung Up Kim, Jun Yong Park, Do Young Kim, Sang Hoon Ahn, Chae Yoon Chon, Kwang-Hyub Han
- Journal of the Korean Liver Cancer Study Group. 2013;13(1):74-79. Published online February 28, 2013
- DOI: https://doi.org/10.17998/jlc.13.1.74
- 1,054 Views
- 4 Downloads
-
 Abstract
Abstract
 PDF
PDF - Hepatocelluar carcinoma (HCC) is the most common primary liver cancer in the world and the most prevalent cancer among patients liver cirrhosis. The management of HCC depends on tumor stage and the degree of liver dysfunction. Patients with intermediate-stage HCC are ineligible for surgical or local ablative treatments. Current treatment guidelines recommend trans-arterial chemoembolization (TACE) for intermediate stage of HCC. However, tumor recurrence after TACE is universal and the survival benefit is relatively small. Hence, new strategies are needed to improve the outcome of HCC patients undergoing TACE. Recently, the combination of target agents with TACE has shown promising overall survival in advanced HCC. It is necessary to investigate new treat strategy how to increase treatment outcome of advanced HCC by new treat strategy.

- A Case of Necrotizing Pancreatitis after Transcatheter Arterial Chemoembolization for Hepatocellular Carcinoma
- Mi Na Kim, Jung Hyun Cho, Young Eun Chon, Beom Kyung Kim, Seung Up Kim, Jun Yong Park, Do Young Kim, Sang Hoon Ahn, Kwang-Hyub Han, Chae Yoon Chon
- Journal of the Korean Liver Cancer Study Group. 2012;12(2):155-159. Published online September 30, 2012
- 556 Views
- 2 Downloads
-
 Abstract
Abstract
 PDF
PDF - Acute pancreatitis is a rare but severe postprocedural complication after transcatheter arterial chemoembolization (TACE) of hepatocellular carcinoma with an incidence of 1.7-4%. The proposed mechanism of this complication is inadvertent embolization through collateral vessels or regurgitation of chemotherapeutic agents to the arteries of other organs. Here, we present a fatal necrotizing pancreatitis case which developed 10 days after TACE, caused by the regurgitation of the chemotherapeutic agents to the pancreas during the procedure. The patient recovered with conservative care at first, but after suffering from several times of recurrent pancreatitis, he died of peritoneal septic shock 5 months after the initial pancreatitis attack.

- A Case of Advanced Hepatocellular Carcinoma which was Supervening with Renal Cell Cancer Cured by Repeated Transarterial Chemoembolization and Sorafenib after Resection
- Bun Kim, Jae Hoon Min, Seung Up Kim, Jun Yong Park, Kwang Hoon Lee, Do Youn Lee, Jin Sub Choi, Young Deuk Choi, Nam Hoon Cho, Young Nyun Park, Sang Hoon Ahn, Kwang Hyub Han, Chae Yoon Chon, Do Young Kim
- Journal of the Korean Liver Cancer Study Group. 2012;12(1):51-57. Published online February 28, 2012
- 471 Views
- 2 Downloads
-
 Abstract
Abstract
 PDF
PDF - Advanced hepatocellular carcinoma (HCC) is difficult to treat and the survival is poor. Here, we present a patient diagnosed as advanced HCC (stage IIIa) which was supervening with early renal cell cancer (stage I). The patient was treated with pre-operational transarterial chemoembolization (TACE) and surgical resection (right hepatectomy, right nephrectomy, and cholecystectomy). Sorafenib were taken continually after surgery. Multiple recurred HCC nodules in remnant liver were detected 2 months later after surgery. Combined treatment modalities including 4 sessions of TACE, and 12 cycles of 5-flurouracil (FU)/carboplatin based hepatic arterial infusional chemotherapy (HAIC) induced complete response. After the diagnosis of advanced HCC, the patient survived 36 months and experienced disease-free status for 19 months.

- A Case of Concurrent Liver Resection and Splenectomy in Patients with Hepatocellular Carcinoma and Decompensated Liver Cirrhosis
- Sung Hoon Kim, JIn Hong Lim, Sang Hoon Ahn, Kyung Sik Kim
- Journal of the Korean Liver Cancer Study Group. 2011;11(2):160-164. Published online September 30, 2011
- 505 Views
- 4 Downloads
-
 Abstract
Abstract
 PDF
PDF - Hepatocellular carcinoma (HCC) develops on chronic liver disease and often accompanies portal hyperternsion. Portal hypertension induces hypersplenism with splenomegaly. Because hypersplenism results in pancytopenia, especially thrombocytopenia, it is not easy to decide the hepatic resection for many surgeons in patients with HCC and hypersplenism. Although liver transplantation is the most ideal treatment for HCC and hypersplenism, liver resection has been performed commonly because of donor shortage. Splenectomy has performed to control intractable varices as a Hassab’s operation (=decongestion of upper gastric marginal veins and splenectomy). Recently, as a development of surgical techniques and equipments, especially laparoscopic surgery, splenectomy has been performed safely and easily. Some studies reported that splenectomy improved the liver function. Splenectomy in patients with HCC expanded the indication of liver resection and increased disease free survival (DFS). However, portal vein thrombosis (PVT) is a one of well-recognized complications of splenectomy and recent prospective study reported the 50% rate of PVT in non-cirrhotic splenectomized patients. Some studies reported that splenectomy with simultaneously or staged liver resection was performed safely without a significant complication and operative mortality. We experienced a case that underwent simultaneously liver resection and splenectomy and then recovered without complication. The further study may be needed to evaluate the role of splenectomy in patients with HCC and hypersplenism.

- A Case of Early and Massive Recurred Hepatocellular Carcinoma in Patients with Ruptured Hepatocellular Carcinoma Underwent Staged-Surgical Resection
- Sung Hoon Kim, Jin Hong Lim, Sang Hoon Ahn, Kyung Sik Kim
- Journal of the Korean Liver Cancer Study Group. 2011;11(2):155-159. Published online September 30, 2011
- 515 Views
- 2 Downloads
-
 Abstract
Abstract
 PDF
PDF - The rupture of hepatocellular carcinoma (HCC) has been uncommon complication. Because the diagnosis of early HCC has been increase due to development of imaging modality and surveillance program, the incidence of ruptured HCC has been decreased. The paradigm of treatment for ruptured HCC has shifted from surgical hemostasis to transcatheteric chemoembolization (TACE) at acute phase. After the control of acute phase, the definitive treatment for HCC is still debate. However, many studies have advocated staged-liver resection. Some studies reported that the patients underwent staged-liver resection showed a similar survival rate compared with survival rate in patient with non-ruptured HCC. The staged-liver resection was usually performed in the patients with well-preserved liver function. The decision of optimal time for surgery after TACE and surgical indications for ruptured HCC after any other primary treatment are controversy. We experienced a cases of early and massive recurrence HCC in patients with well-preserved liver function and the rupture of HCC. The further study may be needed to decide the optimal time of surgery after TACE and surgical indication for rutprued-HCC.

- A Case of Hepatocellular Carcinoma Recurred Extensively during Treatment of Biliary Complication Occurring after Transarterial Chemoembolization
- Hyun Jung Oh, Hana Park, Kwang Hoon Lee, Do Young Kim, Sang Hoon Ahn, Kwang-Hyub Han, Chae Yoon Chon, Jun Yong Park
- Journal of the Korean Liver Cancer Study Group. 2011;11(2):178-184. Published online September 30, 2011
- 519 Views
- 3 Downloads
-
 Abstract
Abstract
 PDF
PDF - Hepatocellular carcinoma(HCC) is one of the cancers with poor prognosis. Transarterial chemoembolization(TACE) has been widely used for treating unresectable HCC. Although TACE is considered as a less invasive and relative safe procedure, severe complications such as hepatic failure, pulmonary embolism, liver abscess, biloma formationcan occur rarely after TACE. These complications sometimes may lead to fatal clinical situation, even death. We reported a case of HCC recurred extensively during treatment of biliary complication after TACE. A 44-year-old male with HCC was admitted due to fever for 3 days after undergoing TACE. Three weeks before the admission, he had been diagnosed with HCC recurrence which presented as two arterial enhancing nodules in MRI and treated with TACE. CT scan showed 7 cm sized air containing fluid collections with necrosis suggestive of liver abscess and 15 cm sized biloma formation. Because the patient was in septic shock at admission, percutaneous catheter drainage was performed with use of broad spectrum antibiotics. After treatment of 3 months, the sizes of hepatic abscess and biloma were remarkably decreased. However, 1 month later, large size tumor recurrence and perihepatic lymph node metastasis were found on a follow-up CT scan. In this case, the cause of rapid growing recurrence after TACE is uncertain, but the development of unanticipated complication seems to affect the progression to poor prognosis. Therefore, early recognization of predisposing factors with proper management would be needed to prevent these serious complications after TACE.

- A Case of Hepatocellular Carcinoma showing Progressive Disease in Systemic Chemotherapy, but Partial Response in Hepatic Arterial Infusion Chemotherapy with the Same Regimen
- Soung Min Jeon, Do Young Kim, Sang Hoon Ahn, Kwang Hyub Han, Chae Yoon Chon, Jun Yong Park
- Journal of the Korean Liver Cancer Study Group. 2010;10(1):44-48. Published online June 30, 2010
- 518 Views
- 0 Download
-
 Abstract
Abstract
 PDF
PDF - Hepatocellular carcinoma (HCC) is the third most common malignancy in Korea. Despite recent advances in the area of HCC, a considerable number of HCC patients require non-surgical treatments and systemic therapies because of poor liver function or intermediate to advanced cancer stages at the time of diagnosis. Unfortunately, chemotherapy for advanced HCC has limited response rates and provides a marginal survival benefit. Several studies have supported potential advantages of hepatic arterial infusion chemotherapy (HAIC), designed to improve chemotherapy benefits by increasing the amount of chemotherapy delivered to the site of the tumor and to minimizes the side-effects of the chemotherapy. However, there hasn’t been any report showing different responses between systemic chemotherapy and HAIC for the same patient. Herein, we report a case of HCC showing progressive disease in systemic chemotherapy, but partial response in HAIC with the same regimen for the same patient with portal vein thrombosis. This case implies HAIC might be alternative option for HCC patient showing ineffective response to systemic chemotherapy, even with the same regimen.

- A Case of Hepatocellular Carcinoma in Young Age Younger than 20 Years Old
- Joo Won Chung, Seung Up Kim, Jun Yong Park, Sang Hoon Ahn, Kwang-Hyub Han, Chae Yoon Chon, Geung-kyu Ko, Jin Sil Seong, Jong Hee Chang, Do Young Kim
- Journal of the Korean Liver Cancer Study Group. 2009;9(1):71-75. Published online June 30, 2009
- 487 Views
- 1 Download
-
 Abstract
Abstract
 PDF
PDF - Hepatocellular carcinoma (HCC) is very rare in young age. Most young patients tend to receive the evaluation only when they experience intractable or persistent symptoms. Therefore, HCC in young patients is often diagnosed at advanced stage and thus, young HCC patients have a worse prognosis than older HCC. However, because young HCC patients show well-preserved liver function than older HCC, they are tolerable to more aggressive treatments. We report a case of advanced HCC in 13-year and 8-month old male who has been a B-viral carrier. Despite the tumor size decreased after concurrent chemoradiation therapy, multiple lung and brain metastases developed. He underwent radiofrequency ablations on lung metastases and gamma-knife surgery on brain metastasis, and he has received systemic and intra-arterial chemotherapy. The screening and early diagnosis of HCC in young age is needed especially for B-viral carrier with a family history of HCC.

- A Case of Curative Resection of Advanced Hepatocellular Carcinoma After Localized Concurrent Chemo-Radiation Therapy
- Wonseok Kang, Ki Tae Yoon, Jun Yong Park, Do Young Kim, Sang Hoon Ahn, Chae Yoon Chon, Kyung Sik Kim, Young Nyun Park, Jin Sil Seong, Kwang Hyub Han
- Journal of the Korean Liver Cancer Study Group. 2008;8(1):98-101. Published online June 30, 2008
- 519 Views
- 3 Downloads
-
 Abstract
Abstract
 PDF
PDF - Most patients with advanced hepatocellular carcinoma (HCC) are not suitable candidates for surgical treatment at the time of diagnosis because of poor liver function, extensive tumor involvement of the liver, vascular involvement, and/or intra/extrahepatic metastasis. We attempted localized concurrent chemo-radiation therapy (CCRT) followed by hepatic arterial infusion chemotherapy (HAIC) in patients having locally advanced HCC with vascular involvement and preserved hepatic function. We report a case of locally advanced HCC patient who became surgically resectable by downstaging after localized CCRT followed by HAIC. Localized CCRT was performed with a total radiation dose of 4,500 cGy (180 cGy × 25 times) and hepatic arterial infusion of 5-fluorouracil (5-FU, 500 mg/day) via implantable port system during the first and the last weeks of the radiotherapy. Following localized CCRT, the patient was scheduled to receive HAIC with 5-FU (500 mg/m2 for 5 hours, days 1~3) and cisplatin (60 mg/m2 for 2 hours, day 2) every 4 weeks. Marked contraction of HCC was noted on follow up computerized tomography (CT) and positron emission tomography (PET) after localized CCRT and HAIC, and subsequently surgical resection with curative aim was performed. The patient is in complete remission status without recurrence to date.


 E-submission
E-submission THE KOREAN LIVER CANCER ASSOCIATION
THE KOREAN LIVER CANCER ASSOCIATION

 First
First Prev
Prev



 Follow JLC on Twitter
Follow JLC on Twitter